early-abdominal-rehab: Sequencing Abdominal Tissue Mobilization with Lymph Drainage for Scar Mobility
early-abdominal-rehab is a strategic approach to improving scar mobility and abdominal comfort through gentle lymph drainage and mindful tissue mobilization.
This guide walks you through practical sequencing, safety notes, and how a spa‑level program can support your healing journey.
You’ll learn how to combine in‑person sessions with an at‑home routine that respects your body’s rhythm, fosters tissue pliability, and avoids overstimulation.
The steps below are designed for people who have completed the initial healing phase and are ready to gently reintroduce mobility that supports comfort, posture, and everyday function.
In our Massachusetts spa practice, practitioners blend proven massage therapy principles with a restorative mindset.
We emphasize gentle touch, expert assessment, and compassionate guidance to help you feel more in control of your healing.
While this guide is informative, it does not replace professional care from your healthcare team.
Always listen to your body and consult your clinician if something feels unsafe or painful.
early-abdominal-rehab Essentials: What It Represents in Scar Mobility and Healing
What makes early-abdominal-rehab distinct for scar mobility
In the early stages of abdominal recovery, focus shifts from raw comfort to controlled movement that supports scar tissue alignment and tissue mobility.
The goal is to cultivate a balanced rhythm between breathing, posture, and gentle manual work that encourages lymph drainage and reduces edema without provoking irritation.
This approach combines soft tissue techniques with education for long‑term comfort.
Clinical insights from industry experts suggest that the right sequence—starting with assessment, then light lymph drainage, followed by gradual tissue mobilization—can help restore natural fascia glide and reduce stiffness as healing progresses.
While numbers vary, the trend toward integrative, non‑invasive strategies continues to grow in 2026, with patients reporting higher satisfaction when care is personalized and paced.
Key components of a well‑designed early‑abdominal‑rehab plan
A well‑designed plan typically includes client education, gentle palpation to identify tight bands, and progressive, low‑load movements.
The emphasis is on safety, comfort, and clear milestones so you know when to stay the course or gently progress.
In practice, practitioners use lymph drainage techniques to encourage fluid movement and minimize swelling, paired with tissue mobilization patterns that support scar mobility without overwhelming your system.
- Begin with a safe assessment of tissue texture and mobility in the abdominal region
- Incorporate light, localized lymph drainage along lymphatic pathways
<liProgress to gentle fascia release and directional tissue mobilization
Sequencing Framework: From Gentle Initiation to Progressive Challenges
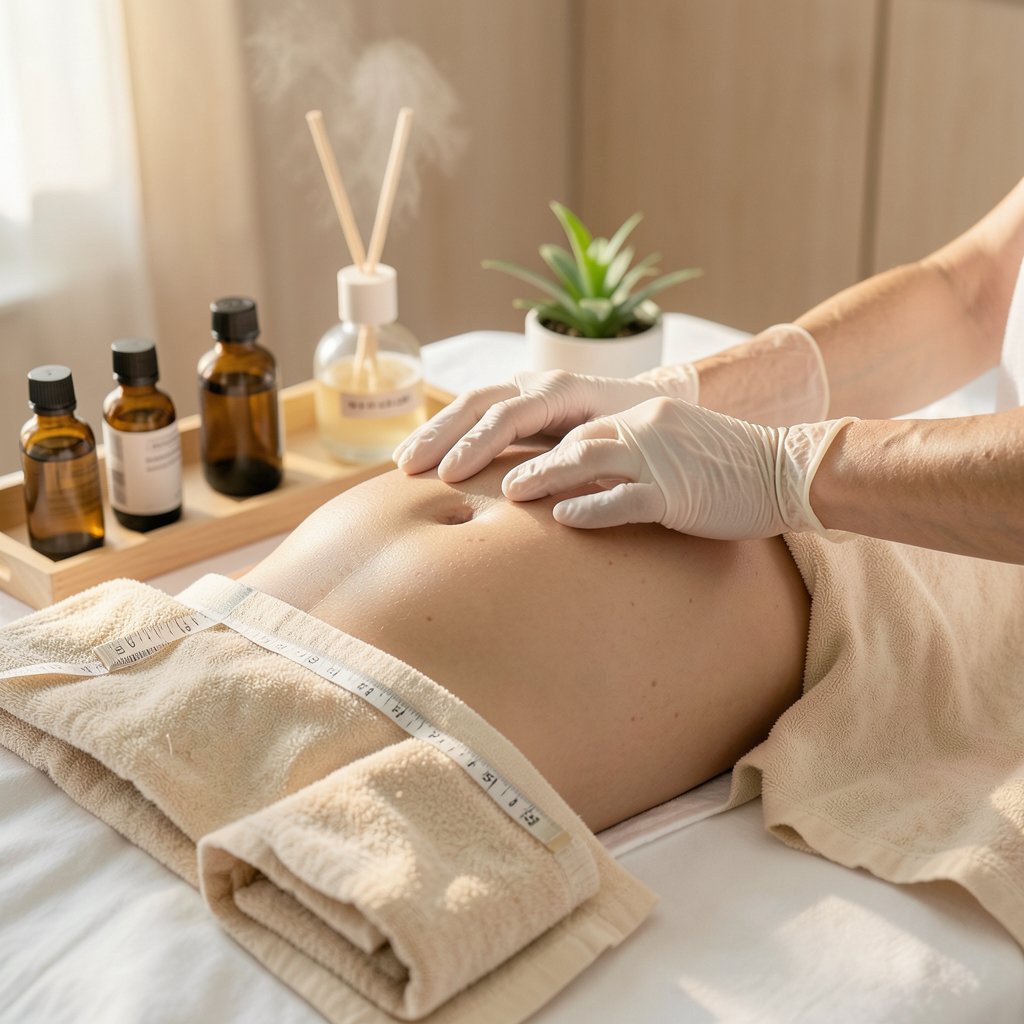
Step 1: Gentle assessment and alignment cues
Start with a quiet, mindful assessment that respects your body’s signals.
A skilled therapist observes breathing patterns, rib cage expansion, and pelvic alignment to determine where scar mobility may be limited.
The goal is to identify areas of tenderness, tissue resistance, and asymmetry without forcing movement.
This initial phase sets the stage for a safe progression and helps tailor the home program you will follow between sessions.
During this stage, simple cues can enhance your experience: slow nasal breathing, relaxed jaw and shoulders, and a comfortable supported position.
These cues help soften the connective tissues and prepare the abdomen for the next steps in the sequence.
A thoughtful, personalized approach fosters trust and reduces anxiety, which is essential for sustained progress.
Step 2: Light lymph drainage techniques to support fluid balance
Ly mph drainage in this context focuses on light, directional strokes that follow natural lymphatic channels.
The intent is to encourage subtle fluid movement and reduce localized edema without inducing soreness.
Therapists emphasize gentle touch and patient feedback throughout the session.
When performed properly, these techniques can contribute to improved tissue pliability and a calmer recovery experience.
Home guidance may include gentle self‑care routines such as soft, shallow strokes along the lower abdomen and gentle diaphragmatic breathing.
The emphasis remains on consistency and listening to your body.
If you notice heightened sensitivity, slow the pace and communicate with your therapist to adjust pressure or duration.
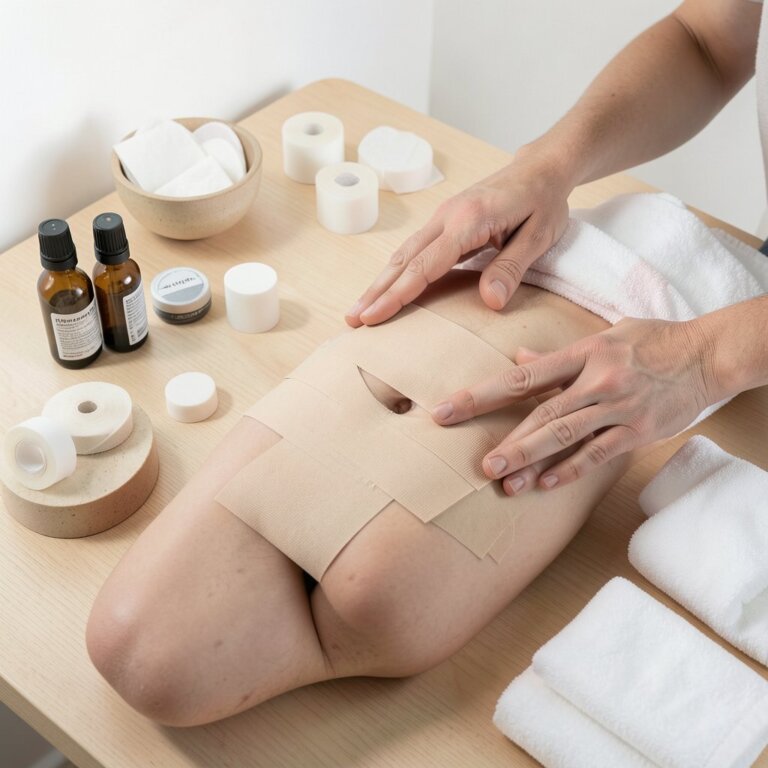
Step 3: Progressive tissue mobilization to restore glide
As comfort increases, practitioners introduce progressive, low‑load tissue mobilization.
Movements focus on improving scar mobility and fascial glide while avoiding abrupt or deep pressure.
The sequence typically expands to organized patterns that respect tissue boundaries and the healing timeline.
The result is a more adaptable abdominal wall that supports everyday activities with less effort.
In a spa setting, clinicians document progress by noting increases in tissue pliability, reductions in reported tightness, and improved postural alignment.
This information informs ongoing adjustments to the plan and helps ensure you stay within your safe recovery window.
Clinical and Home Practice Bridges: In‑Spa Sessions and At‑Home Routines
In‑spa sessions: creating a calm, evidence‑informed environment
In our Best & Beyond Spa locations across Massachusetts, sessions are conducted in a tranquil, private space designed to support relaxation and focused work on the abdominal region.
Therapists combine relaxing massage and therapy with precise lymph drainage and fascia mobilization to help you feel more comfortable and confident in your body.
The environment is clean, vegan, and botanically oriented, aligning with our mission to provide high‑quality wellness experiences.
During each visit, the practitioner explains the plan, demonstrates gentle techniques, and invites your feedback.
The collaborative approach ensures you understand the rationale behind each step, which enhances adherence and satisfaction with the care you receive.
This is an important part of building trust and ensuring your recovery feels supported rather than rushed.
At‑home program: simple, sustainable habits for ongoing progress
A well‑designed home program complements in‑spa care.
Daily, short practices—often 5 to 15 minutes—can reinforce the gains from in‑spa sessions.
Key elements include breathing exercises, light abdominal awareness, and optional self‑massage techniques that maintain tissue mobility between visits.
Consistency matters, and gradual progression is preferred over intensity bursts that may provoke discomfort.
- Gentle diaphragmatic breathing to support abdominal tissue relaxation
- Light, self‑myofascial techniques using clean hands or a soft tool with minimal pressure
- Postural checks and mindful pauses during daily activities to protect new mobility
Tools, Techniques, and Safety Considerations
Essential tools and settings for safe practice
Safe practice hinges on the right environment and the right touch.
In our Massachusetts locations, we prioritize clean, botanical products and a calm setting to reduce stress and support comfort.
Techniques emphasize gentle touch, scar mobility awareness, and preparation for progression as your body welcomes new ranges of motion.
Always consider your body’s signals before increasing intensity.
For home practice, use your hands or a soft tool with light pressure.
Avoid any tools that apply aggressive force or cause pain.
If you experience redness, swelling, or unusual warmth, pause and consult your care team before continuing.
Safety considerations that help sustain progress
Progression should be slow, deliberate, and guided by your sensations.
Prioritize comfort over intensity and maintain open communication with your therapist.
Documenting how you feel after each session helps tailor subsequent visits and ensures your path remains within a comfortable recovery window.
Safety also means avoiding activities that strain the abdominal area during periods of fatigue or illness.
What to expect in a typical session at Best & Beyond Spa
Our sessions balance soothing, restorative work with precise technique.
Expect a calm environment, careful assessment, and a clear plan for progression.
You’ll receive practical guidance you can apply at home, reinforcing a sense of empowerment and control over your healing journey.
This approach resonates with many clients who value a professional, humane, and effective wellness experience in Massachusetts.
Common Mistakes and How to Avoid Them
Mistake #1: Pushing too hard too soon
Overloading the abdominal tissues early in the recovery can lead to tenderness and lingering stiffness.
To avoid this, follow a conservative progression and respect any signs of discomfort.
Your therapist will guide the pace using feedback and observed changes in tissue texture.
Remember, you are training your body, not forcing it to adapt.
To mitigate risk, practice only what you can tolerate and gradually extend the duration and intensity of your movements over weeks, not days.
The key is consistent practice paired with mindful rest when needed.
Mistake #2: Skipping the breathing component
Breath is a powerful ally in abdominal work.
Skipping diaphragmatic breathing can limit tissue relaxation and impede progress.
Integrate slow, full breaths during all movements to support the body’s natural rhythm and reduce stress responses that may hinder mobility.
In sessions, your therapist will emphasize breathing cues that align with each technique.
At home, set a gentle pace and use breath as a guide to pacing and depth of touch.
Mistake #3: Neglecting hydration and nutrition cues
Hydration and sensible nutrition support tissue pliability and lymphatic function.
While not a medical prescription, keeping hydrated and choosing balanced meals can aid your recovery.
Discuss any dietary concerns with a nutrition professional if you have specific health considerations.
Practical tip: drink water consistently throughout the day and place hydration reminders in your daily routine.
Pair meals with easy, anti‑inflammatory choices to promote comfort and mobility.
Measuring Progress and When to Adjust Your Plan
Qualitative indicators of advancement
Progress is often felt as improved comfort, easier deep breaths, and as the abdominal area feels more supple during light touch.
You may notice a broader range of comfortable daytime posture and less stiffness after activity.
Documenting these observations helps your therapist tailor the next steps and keeps your plan aligned with your healing pace.
Monitoring milestones without overreaching
Set realistic milestones such as gradual improvements in tissue mobility, reduced sensitivity to touch, and steadier postural alignment.
If you encounter persistent pain, swelling, or new discomfort, pause and seek guidance from your care team.
The emphasis is on steady, sustainable progress rather than rapid change.
Adjusting the plan based on feedback
Your experiences shape the plan.
Expectations should remain flexible, and the sequence can adapt to your unique healing timeline.
Regular check-ins with your therapist help ensure your home program and in‑spa sessions stay aligned with your goals, values, and comfort levels.
<h2: Why This Approach Resonates in 2026: Evidence, Expertise, and Local Trust
As recovery and wellness continue to intersect in 2026, professionals emphasize personalized care that respects each body’s healing timeline.
Recent industry discussions note that integrative, non‑invasive modalities—like lymph drainage and tissue mobilization—are gaining traction for their potential to support comfort and mobility without reliance on aggressive approaches.
In practice, reputable spa teams, including Best & Beyond Spa, highlight the importance of expert assessment, professional guidance, and a warm, educational approach that helps clients feel heard and empowered.
From a data‑minded perspective, experts indicate that focusing on gentle, progressive movement and fluid management aligns with current best practices for noninvasive care.
These trends underscore why a well‑structured early rehabilitation rhythm can be a meaningful part of a holistic wellness plan.
For Massachusetts residents, the combination of top‑tier spa services and informed therapists offers a trusted environment to explore gentle mobility and scar‑related comfort within a calm, restorative setting.
Incorporating the latest insights from 2026 industry discussions, we emphasize: (1) patient‑centered pacing, (2) clear communication and education, (3) meticulous technique with tissue mobility and lymph drainage, and (4) a seamless bridge between in‑spa care and home practice.
These elements help ensure the experience is both effective and comforting, grounded in real, human needs rather than quick fixes.
Next Steps: Your Guided Path to Comfort and Mobility
Ready to begin or continue your early‑abdominal‑rehab journey? Our team at Best & Beyond Spa in Massachusetts is trained to guide you with warmth, clarity, and evidence‑informed techniques that respect your pace.
Start with a friendly consult to align your goals with a safe, progressive plan that prioritizes scar mobility, tissue pliability, and overall abdominal comfort.
You deserve a restorative experience that values your well‑being and supports your recovery journey through a calm, expert touch.
To learn more about how we can support your recovery with expert lymph drainage and abdominal tissue mobilization, explore our massage and therapy services, then connect with our team for a personalized plan.
We aim to help you feel confident and cared for as you move toward greater mobility and everyday ease.
Frequently Asked Questions
What is the goal of sequencing abdominal tissue mobilization with lymph drainage for scar mobility?
The goal is to gradually improve scar tissue glide, reduce swelling, and restore comfortable movement in the abdominal area. This sequencing supports fascia mobility and posture without overstimulation. It blends gentle lymph drainage with mindful tissue work to create a steadier healing rhythm.
When is it appropriate to begin abdominal tissue mobilization after abdominal surgery?
Begin after the initial healing phase, when the tissue has started to close and there are no signs of active infection. Look for reduced pain, the ability to take full breaths without sharp pain, and tolerance for light touch. Always follow your clinician’s guidance.
How does lymph drainage contribute to improving scar mobility on the abdomen?
Gentle lymph drainage helps move excess fluid away from the healing area, reducing swelling and tissue stiffness. It supports tissue pliability and sets up better conditions for subsequent tissue mobilization. It should be performed with light, non-aggressive techniques.
What does a typical sequencing order look like in early abdominal rehab?
Start with an assessment to identify areas of stiffness and edema, then apply light lymph drainage, followed by gentle tissue mobilization. Breathing coordination and posture work are integrated to support natural fascia glide. Progressions are gradual and paced to avoid irritation.
What safety considerations should I follow when starting the at-home routine?
If pain worsens, swelling increases, or you notice redness or fever, stop and contact your clinician. Use very light touch and avoid aggressive rubbing or deep pressure. Stick to the prescribed routine and progress only as tolerated.
How should I balance in-person sessions with a home program for scar mobility?
Combine spa-level sessions with daily, mindful practice at home to reinforce tissue changes. Use in-person assessments to guide progression and adjust your home routine accordingly. Consistency and listening to your body are key.
What outcomes are common with abdominal tissue mobilization and lymph drainage?
Expect improved scar mobility, more comfortable abdominal movement, and reduced edema. Clients often notice better posture and less tissue stiffness as healing progresses. Long-term benefits include maintained tissue pliability with reduced reactivity.
Do you tailor the approach based on scar age or type?
Yes. Early rehab emphasizes edema control and fascia alignment, while later stages focus more on full tissue mobilization and function. Scar age and tissue type guide pacing, pressure, and exercise selection. Personalization helps optimize comfort and progress.

At Best and Beyond Spa, Day and Davilla are dedicated professionals passionate about wellness and beauty. With expertise in spa day treatments, couples massages, and senior wellness, they provide high-quality, personalized care in a relaxing environment. Their mission is to help clients feel rejuvenated, refreshed, and truly cared for.